In the evenings, a sea breeze cools the stilt houses of Papa village. Families emerge from their homes to sell fish and fresh produce in the centre of town. Boys carry bundles of reed from the shoreline, and workers arrive on trucks from the nearby liquefied natural gas plant, chewing the betel nut that leaves orange-red stains on the roads of Papua New Guinea.
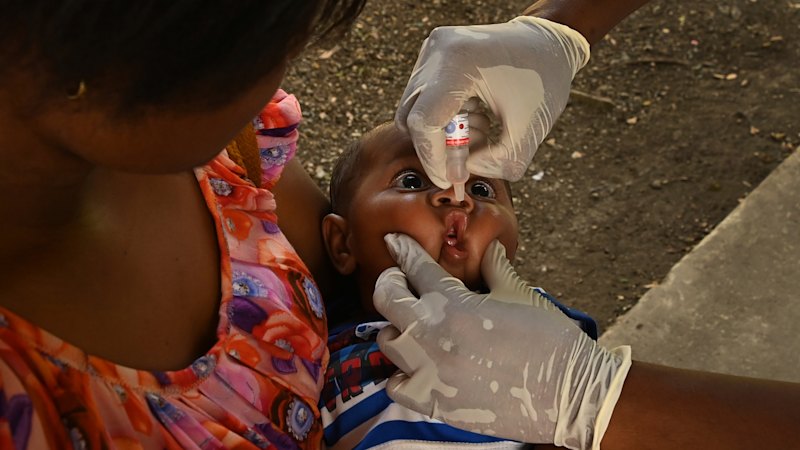
Through the crowd, a woman steps up to a church-issued megaphone. Margaret Kupa is a nurse, not a preacher, but she is here to warn the congregation of an ancient killer.
“Polio is a deadly disease,” she says in Tok Pisin, the common tongue used to communicate across Papua New Guinea’s 800-plus language groups.
“There is a polio outbreak … that’s why children under five need to be vaccinated.”

Kupa is one of hundreds of health workers across PNG responding to the country’s first polio outbreak in eight years. The virus’ discovery last May, in wastewater in the country’s second-largest city, Lae, was another major setback for a country declared polio-free in 2000, and a reminder to its neighbours – including Australia – that eradication remains elusive.
“It’s really a wake-up call,” says Helen Clark, the former prime minister of New Zealand who now chairs Gavi, the international vaccine alliance. “If you drop off numbers from the core vaccination regime, you pave the way for the return of deadly disease.
“I’m old enough to remember being at school in New Zealand with a boy with a withered leg and a brace from polio … we just have to keep our guard up.”
For children in Papa, polio is no distant threat. Just a few kilometres east, in PNG’s Central Province, a child was paralysed by the disease. Another four have suffered infantile paralysis in an outbreak linked to a vaccine-derived variant of poliovirus.
No human case has been detected since September, but immunisation rates remain low and the virus is still showing up in wastewater sampling, meaning thousands of unvaccinated children remain vulnerable.
How vaccine-derived outbreaks take hold
The oral polio vaccine developed by Dr Albert Sabin in the 1950s has been credited with eliminating wild poliovirus in all but two countries.
This vaccine contains a weakened version of the virus which mimics natural infection in the gut. In communities with low immunisation coverage and poor sanitation, this weakened virus can be transmitted between unvaccinated children through contaminated water, eventually mutating over months and years into a poliovirus variant that can cause paralysis.
These vaccine-derived variants have frustrated eradication efforts in recent years, and the Sabin type 2 vaccine has been phased out in favour of a more stable oral vaccine less prone to mutation.
A third vaccination campaign is under way, targeting children under five in four of the 28 provinces. The goal is to vaccinate 95 per cent of children, but health workers must overcome a patchwork road network, a mobile population, and communities sceptical of mass vaccination campaigns following the COVID-19 pandemic.
“Some people, they’re scared,” says Kupa, who runs the health centre in Papa. “When we explain it properly to them, they accept it. If we did not give proper awareness, they are reluctant.”

Garia Ken, 24, doesn’t need any convincing. She took her one-year-old Varnon to be vaccinated during the first vaccination campaign, and will receive another dose at Papa Health Centre when the third campaign begins.
“We are happy that we have these vaccinations brought to our aid post,” she says. “It helps a lot.”
“If there had been large-scale transmission in PNG, the likelihood that we were going to end up picking up something in Australia was relatively high.”
Chris Maher, UNICEF Australia vaccine adviser
The catch-up
At the end of a narrow laneway on the outer fringe of Port Moresby, seven-year-old Leah and her best friend Anna dart back and forth between their neighbouring homes.
Until last year, Leah was still crawling. Her family suspect a polio-like illness she contracted as an infant left her unable to walk, although she was never diagnosed or confirmed by authorities.

“Now, she’s walking, and playing,” says her grandfather, Thomas Orebut, who has been Leah’s primary carer since she was six months old. “I am proud.”
The suspicion that Leah’s childhood illness had affected her development was the primary driver for her family to ensure she was protected against other diseases.
Born in 2019, she missed out on all of her routine childhood immunisations due to pandemic restrictions, and last year’s two polio campaigns offered an opportunity to catch up. Orebut says he will take Leah to get vaccinated again when the campaign visits the area next month.

This is not only a problem for PNG. Globally, an estimated 12.3 million children receiving catch-up vaccinations between 2023 and 2025 were “zero-dose children” who had never been immunised. In Australia, childhood vaccination rates have fallen in every age group for every year since 2020.
Before last year’s outbreak, Papua New Guinea had some of the lowest polio coverage rates in the world; in some provinces, below 40 per cent. Health workers have rafted down rivers, jumped in helicopters, and hiked for days to transport vaccines to some of the country’s most remote communities.
Vaccination rates also remain low in the capital, where thousands of families rely on daily incomes to survive. Many cannot afford time off work to bring their children to be immunised.

Recent large-scale evictions of settlements in Port Moresby have made it even more difficult to track which children have been vaccinated, says Dr Amos Lano, the capital district’s public health director.
“Once people are evicted … you don’t know where they are,” Lano says. “It has been really affecting our [vaccine] programs.”
The latest campaign was delayed by weeks because of issues getting payments to temporary workers, Lano says. A planned nurse strike, avoided with a last-minute pay deal, created another complication for health authorities in the lead-up to the campaign.
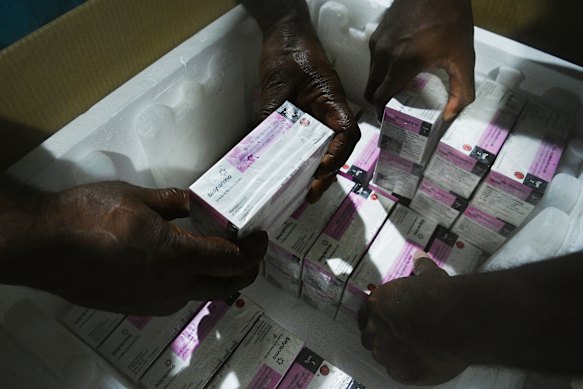
Thousands of volunteers and health workers are involved in the campaign, and many take pride in contributing to an effort that has so far vaccinated more than two million children.
“Giving back to the country – that’s why I’m in this role,” says Lawrence Sihare, a vaccine logistics officer responsible for the national vaccine store in Port Moresby.
“[We] make sure the future of Papua New Guinea is safeguarded.”





‘Would have been a disaster’
In a laboratory at Melbourne’s Peter Doherty Institute, Associate Professor Bruce Thorley examines wastewater samples from thousands of kilometres away.
Thorley’s team was the first to identify the particular strain of type 2 poliovirus circulating in PNG. Testing found it was genetically similar to another outbreak in Indonesia two years before.

The lab has also been sampling wastewater from Cairns since July to ensure the virus does not reach Australian shores. These samples have twice detected the polio vaccine used in PNG, but not the variant virus responsible for the outbreak.
However, vaccine-derived poliovirus has been detected in Australian wastewater in recent years, including an instance linked to an unvaccinated traveller in Melbourne in 2024, and a mid-April detection in Perth wastewater revealed to the public just last week.
Thorley says Australians should not be concerned about polio re-emerging here, but the PNG outbreak is a reminder to stay vigilant.

“Unfortunately, we’re still not completely free of polio,” he says. “We are still at risk of a poliovirus importation into Australia, but we have an effective system of detection and high levels of polio vaccination.”
Chris Maher, a vaccine adviser to UNICEF Australia who chaired the independent advisory group monitoring the outbreak, says the success of the response in limiting transmission has been “enormously protective” for Australia.

“If there had been large-scale transmission in PNG, the likelihood that we were going to end up picking up something in Australia was relatively high,” he says. “Even two, three or four cases would have been a disaster for Australia.”
After the third campaign, PNG will need to sustain its polio surveillance for at least three years before it can guarantee the virus no longer poses a threat. Routine vaccination coverage will also have to improve to avoid another outbreak, Maher says.
“This is an extremely difficult place to operate. They have a history of trying to respond to polio outbreaks, and struggling … because of the complexities of the environment,” he says.
“It’s a very decent success story for a country that you wouldn’t expect to have managed to pull this off.”
This project was supported by a press fellowship from the UN Foundation.